Ejaculatory Ducts
Ejaculatory Ducts are present on each side of the median planeThe lower part of the bladder base comprises of just two ejaculatory duct. Every duct traverses anteroinferiorly via the upper posterior half of the prostate and along the side of prostatic utricle to open in the posterior wall of prostatic urethra on the seminal colliculus (verumontanum) on either side of the opening of prostatic utricle.
Vasa Deferentia (Deferent Ducts)
The Vas Deferens are 2 in number (left and right). It is a thick-walled muscular tube which has the work of carrying spermatozoa from the epididymis to the ejaculatory duct. The length of the vas deferens is around 18 inches (45 cm) along with a narrow lumen with the exception of the terminal part that is sacculated- the ampulla of vas deferens.
Course And Relationships
External Course of Vas Deferens
It starts at the inferior pole of the testis as direct continuance of the duct of epididymis and ascends upward behind the testis and medial to the epididymis. It enters the spermatic cord, where it is located in its posterior part, that is the common site of vasectomy. It goes through inguinal canal and enters the abdominal cavity by going through the deep inguinal ring located lateral to the inferior epigastric artery.
Internal Course of Vas Deferens
It hooks around the lateral side of the inferior epigastric artery and enters backwards and medially across the external iliac vessels and enters the lesser pelvis. In the lesser pelvis, it runs downward and backward on the lateral pelvic wall crossing successively obliterated umbilical artery, obturator nerve, and vessels. Afterward it crosses above and medial to the terminal part of the ureter and makes an angular bend downward and medially. Then, it enters behind the base of the bladder in front of the rectal ampulla and on the medial side of the seminal vesicle. This part of the vas deferens is enlarged and sacculated to create an ampulla which likely keep the semen. Eventually it converges to get to the base of prostate where it joins the duct of the seminal vesicle to create the ejaculatory duct, immediately posterior to the neck of the bladder.
Arterial Supply
The vas deferens is supplied by the following arteries:
- Artery to vas deferens, a branch of superior vesical artery.
- Artery to vas deferens, a branch of inferior vesical artery.
- Artery to vas deferens, a branch of middle rectal artery.
Venous Drainage
The veins from vas deferens join the vesical venous plexus which in turn drains into the internal iliac veins.
Nerve Supply
It’s chiefly by the parasympathetic fibres from the pelvic splanchnic nerves.
Clinical Significance
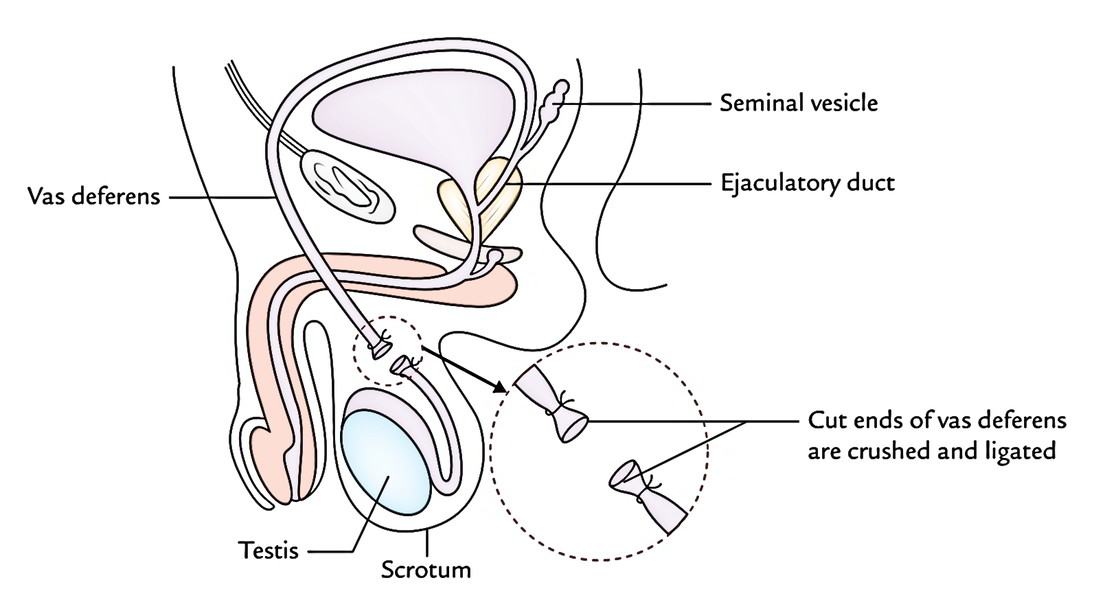
Vasectomy
This is an average procedure of male sterilization. It’s a minor operation done under local anesthesia. In this process, a short section of every vas is excised. The cut ends are squashed and ligated. The vas deferentia are approached via a median incision in the upper part of the scrotum below the penis. Because of this, seminal fluid ejaculated a week after vasectomy, Won’t include sperms and thus pregnancy can not happen. The sperms which continue to be generated go through degeneration and are absorbed in the epididymis.
The development of interstitial cells isn’t influenced, so testes continue to produce testosterone and the individual’s potency isn’t changed.
Reversal of vasectomy is possible. The cut ends are connected and recanalization is done if demanded. Nonetheless, it’s successful in only advantageous cases, i.e., people with less than 30 years of age and if this process is performed inside 7 years of vasectomy.

 (50 votes, average: 4.61 out of 5)
(50 votes, average: 4.61 out of 5)