The eyeball (L. oculus; Gk. ophthalmos) or ball of the eye is an organ that strongly resembles a camera in its structure and is an organ of sight. Additional, such as, for instance, a camera, its interior is black to stop reflection of light.
It’s light sensitive retina and is supplied with a lens system (cornea, lens and refractive media) for focusing images and apparatus for controlling the amount of light acknowledged (the iris diaphragm). The eyeball is an extremely lasting structure, the fluid filled up inside it spreads hydraulic pressure uniformly to keep its shape and its wall enclosing the refractory media, is composed of 3 jackets.
Location
The eyeball is embedded in the fat and takes up the anterior one-third of the orbital cavity. The optic nerve comes from it, a little medial to its posterior post. It’s enclosed in the thin fibrous sheath (Tenon’s fascia), which separates the eyeball from the fat.
Shape and Size
It’s practically spherical in shape and has a diameter of about 24 mm.
Tunics ofThe Eyeball
The eyeball is composed of 3 concentric coatings, viz.
- An outer fibrous coating comprising sclera and cornea.
- A middle vascular coat being composed of choroid, ciliary body and iris.
- An inner nervous coating comprising the retina.
Outer Fibrous Layer ofThe Eyeball
Sclera
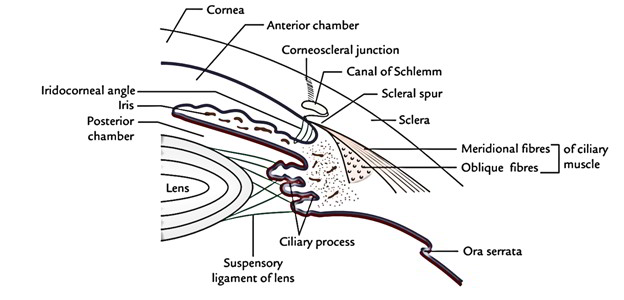
The sclera is the posterior five sixth of the outer coating. It is composed of dense fibrous tissue. It’s opaque and a small portion of it’s viewed as the white of the eye in the palpebral fissure. The sclera is continuous anteriorly with the cornea. The junction between the sclera and cornea is referred to as corneoscleral junction. Just behind the corneoscleral junction, inside the sclera is a circularly running canal referred to as sinus venosussclerae (canal of Schlemm). Posterior to the canal is a triangular projection-the scleral spur-which points forwards and inwards and gives connection to the ciliary muscle. It’s thinnest at the equator and thickest at the back but feeblest at the site of development of optic nerve.
Functions
- Helps to preserve the shape of the eyeball.
- Shields internal structures.
- Gives connection to muscles that move the eyeball.
Structure Piercing the Sclera
Optic nerve pierces the sclera, a little inferomedial to the posterior pole of the eyeball. The perforating fibres of nerve make the area sieve-like (thus referred to as lamina cribrosa).
Posterior ciliary vessels and nerves around the optic nerve.
Anterior ciliary arteries pierce the sclera close to corneoscleral junction.
4 choroidal veins (also referred to as venae vorticosae) pierce the sclera, just behind the equator.
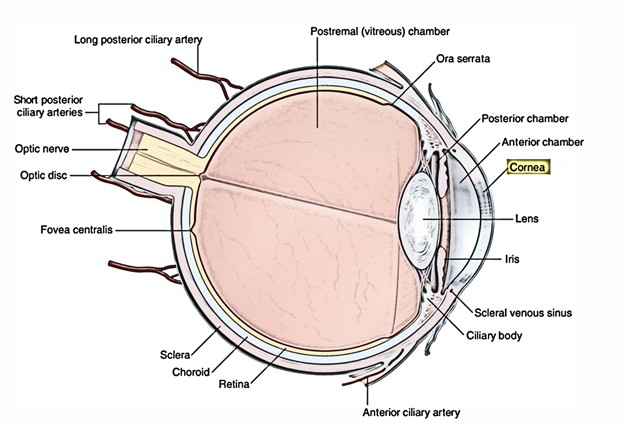
Cornea
The cornea is the anterior 1-sixth of the outer layer. It bulges forwards from the sclera at the corneoscleral junction calledlimbus. It’s clear and much more convex than sclera as it represents the section of a smaller sphere. Its thickness is all about 1 millimeter in the periphery and 0.5 mm at the center.
Features
- It’s avascular and nourished by permeation of nutriments from loops of capillaries at the limbus, aqueous humour and lacrimal fluid.
- It not only allows the light to go into the eye but also reflects the entering light.
- It’s highly sensitive and supplied by the ophthalmic division of trigeminal nerve.
The nerves of cornea create the afferent limb of the corneal reflex (closing of the eyelids on excitement of the cornea).
Structure
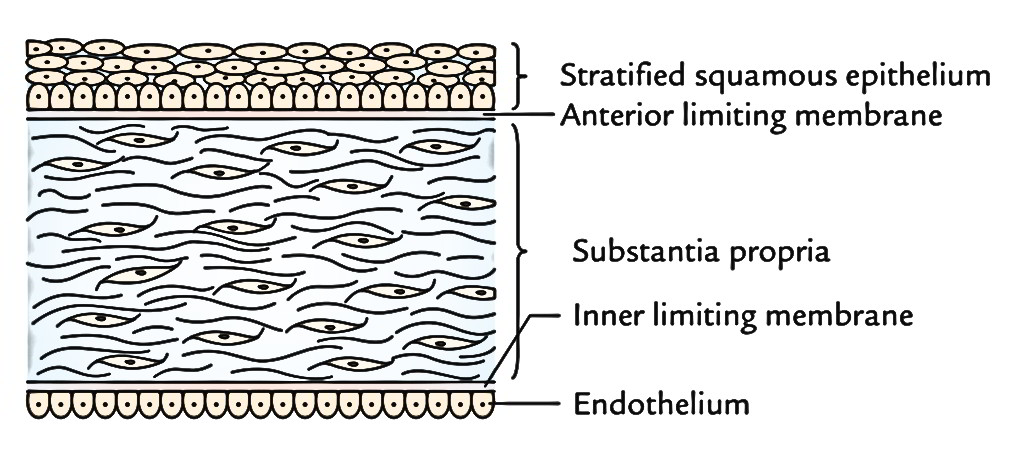
It contains 5 layers, from outside inwards these are as follows:
Corneal epithelium: It is composed of non-keratinized stratified squamous epithelium.
Anterior limiting membrane (or Bowman’s membrane): It’s made up structureless homogeneous mass with no elastic fibres.
Substantiapropria (corneal stroma): It’s created from about 200-250 lamellae of fine collagen fibres, which cross every other at right angles to create corneal spaces.
Flattened fibroblasts are found between the lamellae.
The transparency of cornea is a result of exact lattice arrangement of its lamellae embedded in the ground substance.
Posterior limiting membrane/Descemet’s membrane: It ismade up of structureless homogeneous mass consisting of elastic fibres.
Endothelium: It is composed of a single layer of low cuboidal cells.
Clinical Significance
The periphery of the cornea often exhibits a whitish ring in elderly individuals, owing to fatty degeneration. This whitish ring is called arcussenilis.
Plastic lens: The central part of the cornea gets oxygen from the outside air. Thus, the soft plastic contact lenses worn for long intervals must be permeable to the air in order that oxygen can reach the cornea.
Corneal opacity: The injury to cornea can cause opacity that could interfere with vision. The most frequent injuries of the eye are the wounds or tears of the cornea caused by foreign bodies.
Corneal graft: The normal dearth of vascularity and of lymph vessels accounts for the great success of corneal grafts. The cornea is successfully grafted from 1 man to the other.
The corneal reflex is evoked medically by soft touching of the cornea with wisp of cotton wool. As the cornea is touched both the eyes are closed.
Pathway: Ophthalmic nerve (afferent limb) ^ Principal sensory nucleus of trigeminal nerve ^ Reticular formation ^ Both the facial nerves (efferent limbs).
Middle Vascular Layer ofThe Eyeball
The middle jacket is usually referred to as vascular coating for the reason that it includes majority of the blood vessels of the eyeball. It’s often referred to as uveal tract by the clinicians. This jacket also includes a large number of melaninconsisting of cells. It includes 3 parts; from behind forwards these are: choroid, ciliary body and iris. These 3 parts collectively create uvea or uveal tract.
Choroid
The choroid is the posterior part of the vascular layer of the eyeball. It’s brownish, thin and highly vascular membrane lining the inner outermost layer of the sclera. Anteriorly, it’s linked to the iris by the ciliary body and posteriorly, it’s pierced by the optic nerve.
- Arteries: They’re originated from short ciliary arteries, which pierce the sclera around the optic nerve.
- Veins: They’re ordered in the form of whorls, which converge to create the 4 or 5 venae vorticosae, which pierce the sclera just behind the equator to open into the ophthalmic veins.
The inner outermost layer of the choroid is securely connected to the retina and nourishes the rods and cones of the retina by diffusion.
Structure
It is composed of 4 layers (from outside inwards), viz.
- Suprachoroid lamina (lamina fusca): It is composed of loose network of elastic and collagen fibres and is traversed by long posterior ciliary vessels and nerves.
- Vascular lamina: It includes loose areolar tissue and pigment cells. It includes branches of short posterior ciliary arteries and veins, which converge in whorls to create four or five venae vorticosae, which pierce the sclera and drain into ophthalmic veins.
- Capillary lamina (capillary layer of choroid): It contains fine network of capillaries, which nourish photoreceptors of the retina (rods and cones) by diffusion.
- Basal lamina (membrane of Bruch): It’s a thin transparent membrane that is securely connected to the pigment cell layer of the retina.
The past 3 layers create the choroid appropriate that is divided from sclera by suprachoroid lamina.
In some creatures like cat, tiger, lion, etc. the specialized cells of choroid create a revealing media named tapetum, which generates greenish glare in the eyes of these creatures in the nighttime.
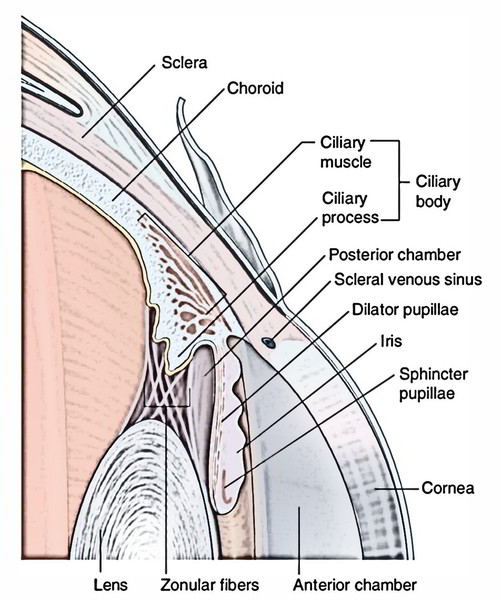
Ciliary Body
The ciliary body is the thickening in the vascular tunic. It’s constant with the choroid behind and the iris in front. It’s situated posterior to the corneoscleral junction in front of the oraserrata of the retina.
The ciliary bodies suspend the lens via suspensory ligaments. Parts of the Ciliary Body.
The ciliary body is triangular in cross section, thick in front and thin behind. The ciliary body is composed of (a) ciliary ring, (b) ciliary processes and (c) ciliary muscle.
Ciliary ring is an outer fibrous ring that is constant with the choroid, viz.
- Ciliary processes are a group of 60-90 folds on the inner aspect of the ciliary body. They may be arranged radially between the ciliary ring and the iris. The grooves between the processes supply connection to the fibres of suspensory ligament of the lens.
- The ciliary processes are a complex of capillaries and cuboidal epithelium, which secretes aqueous humour. The ciliary processes may be compared to choroidal plexus of the brain ventricles affected in the secretion of CSF.
The ciliary muscle is a small unstriped (smooth) muscle mass being composed of primarily 2 types of fibres, viz.
- Outer radial fibres.
- Inner circular fibres.
Functions
Its principal function would be to focus the lens for near vision. The ciliary muscle as a whole acts as a sphincter, so, when its muscle fibres, both radial and circular contract, the choroid is pulled in the direction of the lens reducing the tension on the suspensory ligaments. This enables the lens to assume a more spherical create due to its own elastic nature. Now lens can cause more refraction necessary for lodging.
Iris
The iris is a contractile diaphragm between the cornea and the lens. An opening in its center is referred to as the student. The iris is connected at its periphery to the middle of the anteriorsurface of the ciliary body. Peripheral to this connection the ciliary body and narrow rim of sclera create the iridocorneal angle.
Structure
The iris is composed of 4 layers; from before backwards, all these are as follows:
- An anterior mesothelial lining.
- A connective tissue stroma consisting of pigment cells and blood vessels.
- A layer of smooth muscle, which includes 2 parts.
- Constrictor pupillae-an inner (near the margin of the pupil) part made of circular fibres.
- Dilator pupillae-a peripheral part composed of radial fibres.
Nerve Supply: Constrictor pupillae is supplied by the parasympathetic fibres and dilator pupillae by the sympathetic fibres.
Activities: The constrictor and dilator pupillae constricts and dilates the pupil, respectively.
A posterior layer of pigment cells that is continuous with the ciliary part of the retina.
Inner Nervous Jacket of The Eyeball (Retina)
The retina is the innermost layer of the eyeball. It is composed of 2 layers, viz.
- An outer pigment layer.
- An inner sensory layer.
The space between both layers includes a gummy substance that glues the 2 layers.
The retina is present between the choroid and the hyaloid membrane of the vitreous. The retina declines in thickness from behind forwards. Anteriorly, it presents an uneven border termed oraserrata.
Structure
The outer layer of the retina is insensitive to light and created from pigmented cuboidal epithelium.
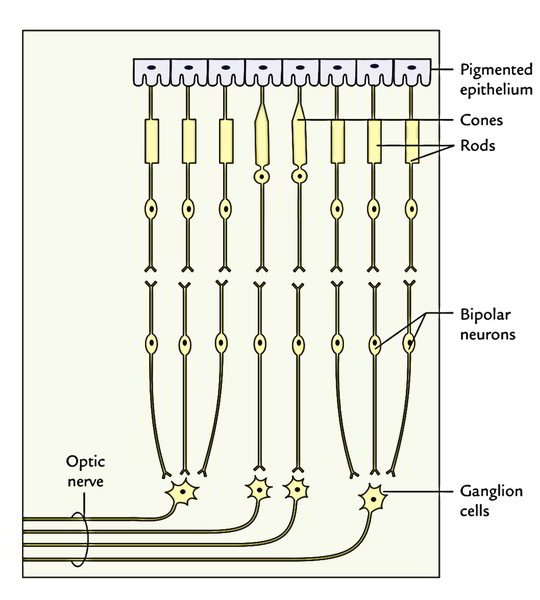
The inner sensory layer of the retina is sensitive to light and is composed of photoreceptors cells named rods and cones; in addition to numerous relay neurons, viz. bipolar neurons and ganglion cells. The really thin non cellular continuance of the retina in front of the oraserrata covers the ciliary body and iris. So the photosensitive part of the retina lines the inner outermost layer of the eyeball posterior to the ciliary body. The nerve fibres originating from its ganglion cells covers inner surface and gather in the inferomedial region, where they pierce the outer 2 coatings of eyeball and come as the optic nerve.
Histologically, the retina consists of following 10 layers:
- Outer pigmented layer.
- Layer of rods and cones (photoreceptor cells).
- External restricting membrane.
- Outer nuclear layer (Cell bodies of rods and cones).
- Outer plexiform layer.
- Inner nuclear layer (Cell bodies of bipolar neurons).
- Inner plexiform layer.
- Ganglion cell layer.
- Nerve fibre layer.
- Internal limiting membrane.
Blood Supply
The deeper part of the retina, i.e., up to the bipolar neurons is supplied by the central artery of the retina (a branch of the ophthalmic artery), while the superficial part of the retina up to the rods and cones is nourished by diffusion from the capillaries of the choroid.
Venous Drainage
It’s by central vein of the retina, which empties into the cavernous sinus.
Development ofThe Retina
The retina grows from a hollow outgrowth the optic vesicle from diencephalon of archaic brain. The optic vesicle becomes invaginated to create the optic cup, being composed of 2 layers of cells. The outer layer differentiates to create the pigment cell layer and the inner layer differentiates to create the nerve layer. The nerve layer creates the remaining layers of the retina with photoreceptor cell (rods and cones) outermost, i.e., next to pigment cells. The ganglion cells are innermost. Consequently light has to go through them to excite the rods and cones.
The 2 layers of optic cup stay different during embryonic interval but fuse afterwards during early fetal period with potential space between the 2. Consequently in retinal detachment, the plane of cleavage is between pigment cell layer and nerve layer.
Clinical Significance
Retinal detachment: In retinal detachment there’s separation of 2 layers of the retina (i.e., pigment and nerve layers).
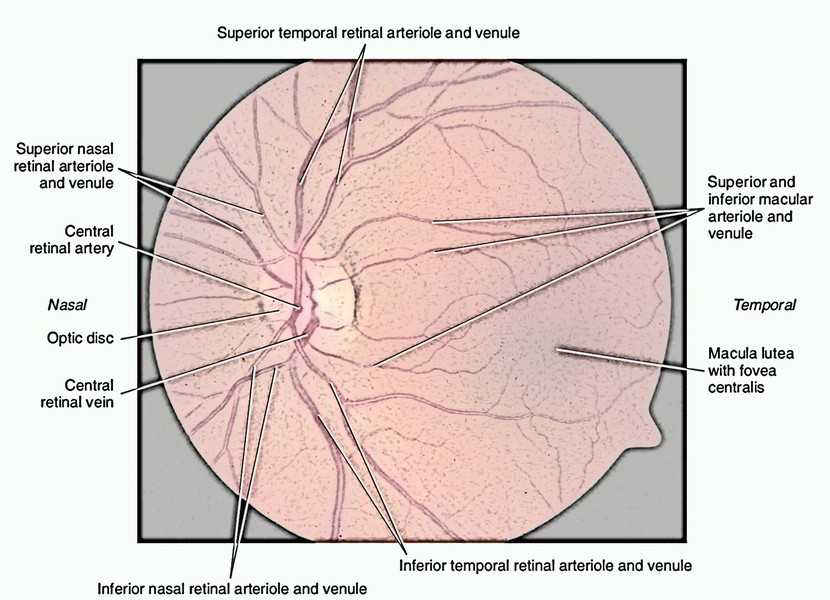
Look of the retina as observed via an ophthalmoscope: The posterior region of retina (fundus) can be analyzed by an ophthalmoscope, a process referred to as fundoscopy (funduscopic evaluation). These features are detected :
Macula lutea, a light yellowish area near the posterior pole.
- It’s roughly 4 millimeters in diameter. A small pit (1.5 millimeters in diameter) in its centre is named fovea centralis that is the point where light is normally focused.
- The fovea is the portion of retina with maximum concentration of cone receptors, thus the site of best visual acuity, i.e., the ability to see the fine images (sharpest eyesight).
Optic disc (1.5 millimeters in diameter), a white spot about 3 mm medial to the macula. The depressed area in the centre is referred to as physiological cup.
- The nerve fibres from retina meet and go through this region (optic disc) of the eyeball to create the optic nerve. The blood vessels of retina also go through this spot.
- Since there are not any photoreceptor cells in the optic disc, it doesn’t react to the light. Thus, the optic disc is also named blind spot.
The central artery of the retina enters the eye via the centre of the optic disc. It splits into superior and inferior branches. Every of them farther splits into temporal and nasal branches. The retinal veins follow the arteries. The branches of the central artery of retina are viewed radiating over the borders of the optic disc. They’re smaller and softer than veins. At points where they cross veins, the vein wall can be observed via the artery.
The normal optic disc appears as a cup shaped area lighter compared to the surrounding area (fundus). The borders of the disk are sharp and well defined.
The blockage of the optic disc from increased intracranial pressure is termed papilledema where the optic cup is clouded and the disk margin is clouded.
The fovea centralis is the thinnest part of retina and itssize is comparable to optic disc.
Arterial Supply ofThe Eyeball
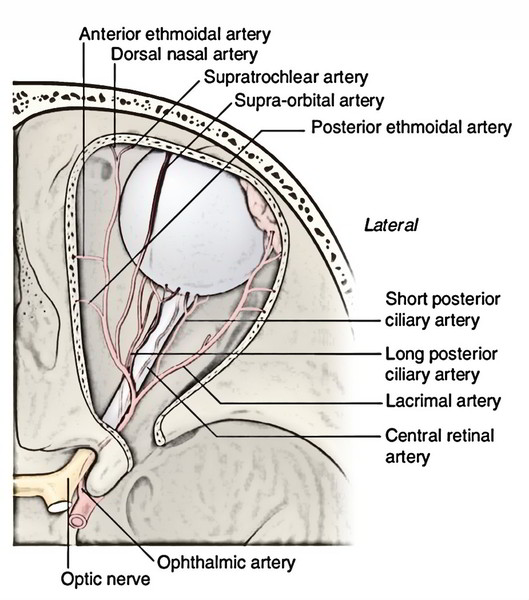
The eyeball is supplied by the following arteries:
- Central artery of the retina.
- Long and short posterior ciliary arteries.
- Anterior ciliary arteries.
In the region of ciliary body, a major arterial circle is composed by the anastomosis between long posterior ciliary artery and anterior ciliary artery. From major arterial circle the vessel enters centripetally and anastomoses close to the pupillary margin to create the minor arterial circle.
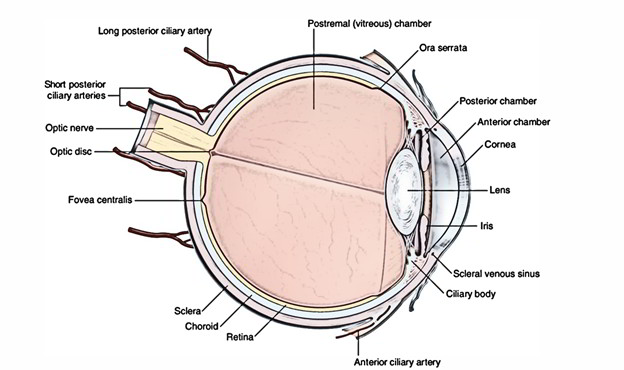
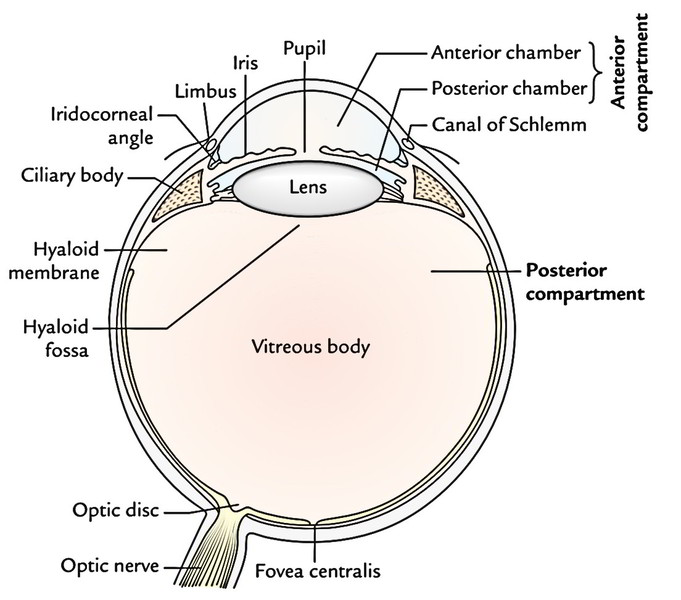
Compartments of the Eyeball
The inner part of the eyeball is split into 2 compartments by the lens: a small anterior compartment in front of the lens and a large posterior compartment supporting the lens:
Anterior compartment: It’s split into 2 chambers: a smaller anterior chamber and a bigger posterior chamber.
The anterior chamber is located between the iris and cornea and posterior chamber between iris and lens. Both compartments communicate with every other via pupil.
The 2 chambers are filled up with an aqueous humour, which helps in keeping the intraocular pressure. The aqueous humour is rich in ascorbic acid, glucose and amino acids. It nourishes the cornea and the lens that are otherwise avascular.
Circulation of aqueous humour: The aqueous humour is secreted in the posterior chamber by the ciliary processes. From here it enters into the anterior chamber via the pupil. Here it goes through the spaces in the iridocorneal angle, found between the fibres of ligamentumpectinatum and after that goes into the canal of Schlemm, from where it’s emptied by the anterior ciliary veins.
Posterior compartment: It’s behind the lens and considerably bigger compared to the anterior compartment (containing 4-fifth of the eyeball). It’s surrounded just about entirely by the retina and is filled up with colorless, clear jelly like substance referred to as vitreous humour/ vitreous body. The vitreous humour is enclosed in a fragile hyaloid membrane. Anteriorly, the hyaloid membrane creates a depression the hyaloid fossa where rests the lens. The vitreous humour helps in keeping intraocular pressure and for that reason the shape of the eyeball. Additionally, it holds the lens and the retina in position. The hyaloid canal goes from optic disc to the lens. The canal indicates the site of the hyaloid artery in the fetus. The hyaloid artery is a continuation of central artery of the retina which vanishes 6 weeks before arrival.
Clinical Significance
Glaucoma
If the drainage of aqueous humour is obstructed, there takes place an abnormal upsurge in the intraocular pressure-a condition referred to as glaucoma. Because of this, there’s intense pain in the eye because of pressure on the highly sensitive cornea.
The glaucoma can cause assortment of visual problems, viz. blindness because of compaction of retina and its blood supply.
The intraocular pressure which normally is about 15 mmHg can be quantified on anesthetized cornea (tonometry).
Lens
The lens is an uncommon biological structure. It’s a clear, biconvex body, 1 cm in diameter and 4 millimeters thick, set between the anterior and posterior compartments of the eyeball.
External Features
The lens presents the following external features:
- Anterior and posterior surfaces.
- Anterior and posterior poles.
- A circumference-the equator.
The line joining the anterior and posterior poles is termed the axis of the lens.
Structure
The lens is enclosed in a translucent elastic capsule. Anteriorly deep to capsule is located capsular epithelium. In the centre, the epithelium is created from a single layer of cuboidal cells. The cells at periphery prolongate to generate lens fibres. These fibres get arranged concentrically and create the lens substance. The centre (nucleus) of the lens is composed of earliest fibres. Here the lens fibres lose their nuclei and organelles. Because of this, an unique group of proteins named crystallines be located in the centre. The centre of the lens is, thus, hard. The periphery of the lens (cortex) is soft because it’s created from more lately created fibres.
Suspensory Ligaments ofThe Lens (ZonuleofZinn)
The lens is suspended between the anterior and posterior compartments of the eye by suspensory ligaments of the lens. These ligaments stretch from ciliary body to the lens capsule largely in front.
Clinical Significance
Presbyopia (Brief Eyesight)
The lens plays a significant part in adjustment. The lens consumes much of the ultraviolet light and becomes increasingly yellowish with age. It also becomes more challenging with age. As an outcome of which the power of adjustment is decreased in old age creating a clinical condition named presbyopia.
Cataract
The opacity of the lens is called cataract. With increasing age and in specific disease states, the lens becomes opaque. The raising opacity results in raising visual impairment. This can be medicated surgically by excision of opaque lens and replacement with an artificial lens.
Functions of the Eye
The key purpose of the eye is focusing of light waves and stimulation of photoreceptors of the retina. This demands 5 basic processes, viz.
- Transmission of light waves via clear media of the eyeball.
- Refraction (bending) of light waves via distinct refractive media of different densities.
- Adjustment of the lens to focus the light waves.
- Regulation of amount of light going into the eye via pupil by iris diaphragm.
- Convergence of eyeballs.
The stimulation of photoreceptors of retina creates action potentials which are relayed via the optic path-means to the visual cortex of the brain, where image is composed. The visual impairment may result if any 1 or more of these processes don’t work correctly.
Refractive Media of the Eye
These contain:
- Cornea (quite refractive but not flexible).
- Aqueous humour.
- Lens (refractive and flexible).
- Vitreous humour/vitreous body.
All these media collectively create the refractive equipment of the eye.
Majority of the refraction by eye happens at the anterior outermost layer of the cornea (not in the lens as usually believed).

 (52 votes, average: 4.83 out of 5)
(52 votes, average: 4.83 out of 5)