Structure
The lacrimal apparatus jointly created by the structures concerned with secretion and drainage of lacrimal (fluid of tears) fluid.
The lacrimal apparatus is composed of the following structures:
- Lacrimal gland
- Ducts of lacrimal gland
- Conjunctival sac.
- Lacrimal puncta.
- Orbital part of lacrimal gland
- Palpebral part of lacrimal gland
- Levator palpebrae superioris
- Lacrimal punctum
- Lacrimal canaliculi.
- Lacrimal sac.
- Nasolacrimal duct.
Lacrimal Gland
It is a J-shaped serous gland It is made up of upper large orbital part and lower small palpebral part. Both parts are constant with every other around the lateral margin of the levator palpebrae superioris.
Situated in the lacrimal fossa in the anterolateral part of the roof of the bony orbit and orbital part is almond shaped.
The palpebral part is situated in the lateral part of the upper eyelid below the levator palpebrae superioris and goes up to the superior fornix of conjunctiva and is one-third of the size of the orbital part.
Ducts of the Lacrimal Gland
The ducts of lacrimal gland are roughly 12 in number, about 4 or 5 from orbital part and 6-8 from palpebrae part. They open into the lateral parts of the superior fornix of the conjunctival sac.
Lacrimal gland secretes the lacrimal (tear) fluid and its ducts express it to conjunctival sac.
About 1 ml of lacrimal fluid is secreted per day. Half of it evaporates and staying half is drained into lacrimal sac.
Functions of Lacrimal Fluid
- Flushes the conjunctiva and keeps the cornea damp.
- Gives nourishment to cornea.
- Functions to express emotions- spilling of tears during despair and sorrow.
- Prevents infection (for it includes bactericidal lysozyme).
Accessory lacrimal glands (glands of Krause): All these are extremely small serous glands found underneath the palpebral conjunctiva near the fornices. They’re about 35-40 in the upper eyelid and 6-8 in the lower eyelid.
Arterial supply: It’s by lacrimal branch of ophthalmic artery. Venous drainage: It’s by ophthalmic veins.
Nerve Supply of lacrimal gland: The lacrimal gland is supplied by parasympathetic (secretomotor), sympathetic and sensory fibres via lacrimal nerves.
The following nerves supply the lacrimal gland:
1. Parasympathetic (secretomotor) supply of the lacrimal gland: The pathway of parasympathetic innervation is as follows:
- The preganglionic parasympathetic fibres originate from lacrimatory nucleus in the pons and pass successively via nervus intermedius, geniculate ganglion, greater petrosal nerve, nerve of pterygoid canal to get to the pterygopalatine ganglion where they relay.
- The postganglionic fibres originate from the cells of the pterygopalatine ganglion and pass successively via maxillary nerve, zygomatic nerve, zygomaticotemporal nerve and lacrimal nerve to reach the lacrimal gland
2. Sympathetic (vasomotor) supply.
3. Sensory Supply: It’s by sensory fibres of lacrimal nerve, a branch of ophthalmic division of trigeminal nerve.
Conjunctival Sac
It’s a potential space between palpebral and bulbar conjunctiva.
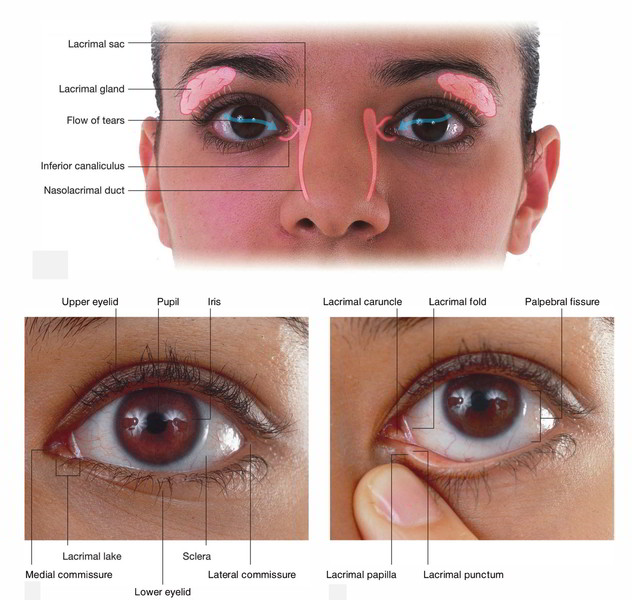
Lacrimal Puncta
All these are small openings on the eyelid margins.
At the junction of these, there’s a small conical projection termed lacrimal papilla surmounted by a miniature aperture named lacrimal punctum. The lacrimal papilla faces inwards in the direction of the lacus lacrimalis.
Lacrimal Canaliculi
There are just two lacrimal canaliculi, superior and inferior in upper and lower eyelids, respectively. Every canaliculus measures about 10 millimeters in length and starts at lacrimal punctum. The superior canaliculus at first runs upwards and after that bends downwards and medially along the complimentary margin of the eyelid to open into the lacrimal sac.
The inferior canaliculus at first runs downwards and after that bends upwards and medially to open into the lacrimal sac. At the bending every canaliculus presents a small dilatation referred to as ampulla.
Key Points
- Both canaliculi converge medially in the direction of the lacrimal sac into which they open individually but occasionally by a common dilated stalk.
- Canaliculi be located behind the medial palpebral ligament.
- Canaliculi are lined by stratified squamous epithelium and include elastic fibres in their own walls, which make them dilatable by the probe.
- A few muscle fibres originated from lacrimal part of orbicularis oculi are arranged circularly around the base of the lacrimal papilla and apply sphincteric actions.
Lacrimal Sac
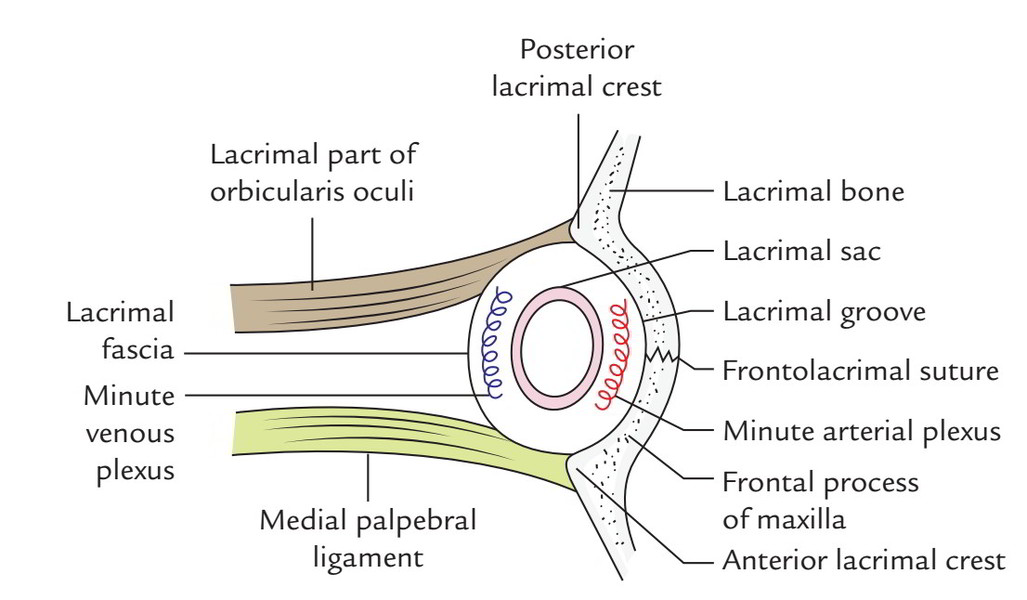
It’s the upper dilated end of the nasolacrimal duct. It’s situated in the deep lacrimal groove bound by posterior lacrimal crest of lacrimal bone and anterior lacrimal crest of frontal process of the maxilla. The sac isenclosed in the lacrimal fascia; when distended the lacrimal sac is all about 15 mm long and 5-6 mm in breadth. It’s divisible into 3 parts: fundus, body and neck from above downwards. The narrow neck becomes constant with nasolacrimal duct.
Connections:
- Anteriorly: Medial palpebral ligament.
- Posteriorly: Lacrimal part of orbicularis oculi (which originates from crest of lacrimal bone and from lacrimal fascia).
- Laterally: Lacrimal fascia that is originated from orbital periosteum and tiny plexus of veins.
- Medially: Lacrimal groove and tiny arterial plexus.
Nasolacrimal Duct
It’s a membranous canal, about 18 mm long, stretching from neck of lacrimal sac to the anterior part of inferior meatus of the nose. It’s lodged in the bony canal created by maxilla, lacrimal bone and inferior nasal concha. Its lower opening presents an incomplete mucous fold named lacrimal fold or valve of Hasner, which keeps the air from blowing the duct into the eye when one smashes his nose to clean nasal secretions.
Variables Helping the Drainage of Tears
Drainage of tears takes place by following means:
- Flashing movements of eyelids.
- Capillary action of the film of the fluid.
- Contraction of lacrimal part of orbicularis oculi resulting in distension of lacrimal sac.
Development of Nasolacrimal Duct and Lacrimal Sac
The nasolacrimal duct grows from a solid cellular ecto-dermal cord, which creates along the nasolacrimal groove, the line of fusion of maxillary and lateral nasal processes. Afterwards, the cord become submerged below the surface ectoderm and becomes canalized during the third month to create the nasolacrimal duct. The upper end of the duct wiholes to create the lacrimal sac, which develops secondary relation to the conjunctival sac by lacrimal canaliculi.
Clinical Significance
When lacrimal gland does not secrete lacrimal fluid as in case of Bell’s palsy, the artificial tears are instilled in the eye at regular periods to forbid the cornea from drying and desiccation.
Ducts from orbital part traverse the palpebral part to open into conjunctival sac. Consequently, removal of palpebral part of gland is functionally comparable to removal of the complete lacrimal gland
The removal of whole lacrimal gland doesn’t result in dryness of conjunctiva because it’s kept damp by the secretions of accessory lacrimal glands.
Epiphora: It’s an overflow of tears from conjunctival sacover the cheeks. It might happen because of:
- Excessive secretion of tears (hyperlacrimation) follow-ing consumption of hot food or psychological outbreak, or.
- Obstruction in lacrimal passages, viz. lacrimal punctum, lacrimal canaliculi, lacrimal sac and nasolacrimal duct, or.
- Eversion of lower eyelid (ectropion), therefore that of lacrimal papilla and lacrimal punctum as a result of laxity of orbiculi oculi in old age or loss of its tone on account of paralysis.

 (64 votes, average: 4.75 out of 5)
(64 votes, average: 4.75 out of 5)