Liver (Greek hepar. liver) is the largest gland of the body, inhabiting much of the right upper part of the abdominal cavity. Just like in pancreas, the liver is also composed of both exocrine and endocrine parts. The liver performs a broad range of metabolic processes essential for homeostasis, nourishment, and immune response. Some of its important functions are:
- It secretes bile and stores glycogen.
- It synthesizes the serum proteins and lipids.
- It detoxifies blood from endogenous and exogenous materials (example, toxins, drugs, booze, etc.) that goes into the circulation.
- It creates hemopoietic cells of all types during fetal life.
Location
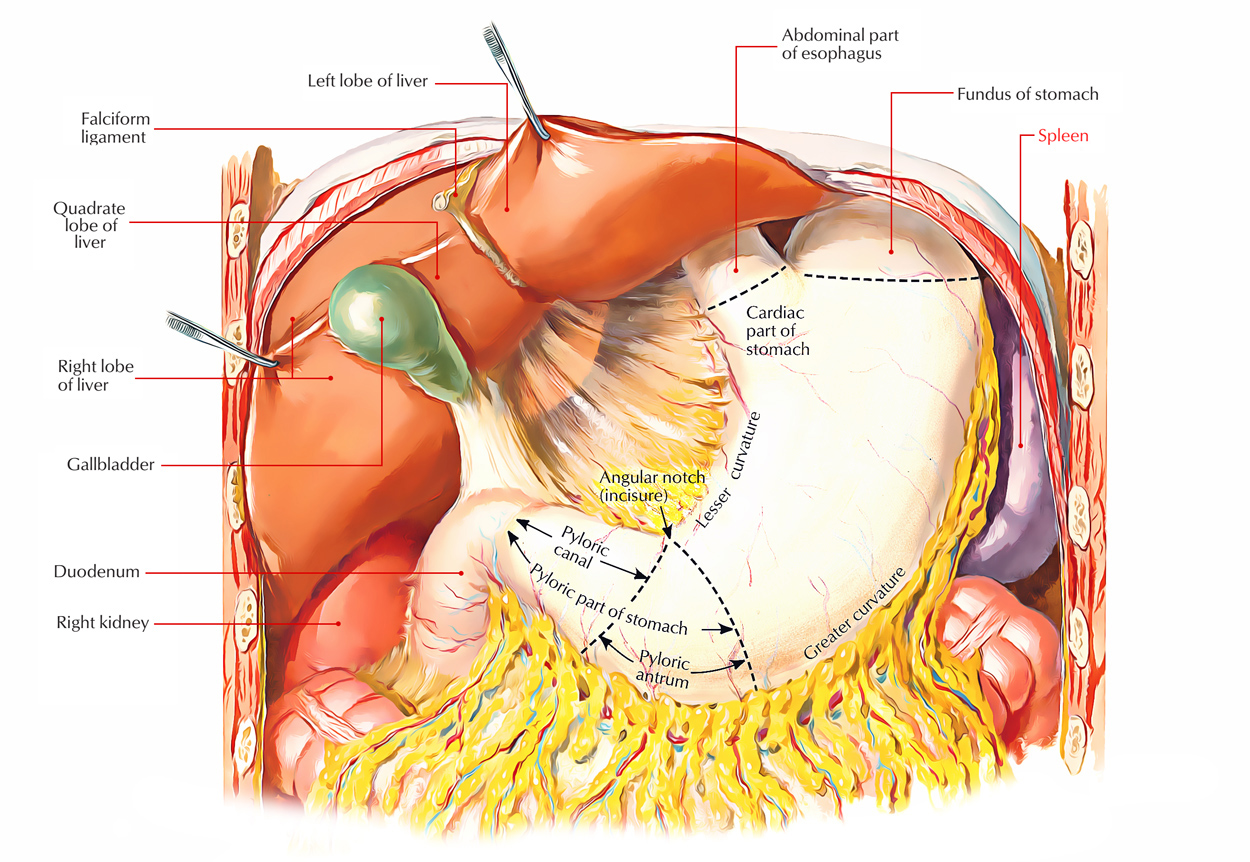
Liver: Location
The liver virtually entirely takes up the right hypochondrium, upper part of the epigastrium, and part of the left hypochondrium up to the left lateral (mid clavicular) line. It is located mainly under cover of the ribs and costal cartilages immediately below the diaphragm. It stretches upward under the rib cage as far as the 5th rib anteriorly on the right side (below the right nipple) and left 5th intercostal space anteriorly on the left side (below and medial to the left nipple).
In the midline, the upper border is located at the level of the xiphisternal joint. The sharp inferior border crosses the midline in the level of transpyloric plane (at the level of L1 vertebra).
The liver is quite a bit bigger in newborn and young kids on account of its hemopoietic function in fetal life, and takes up 2/5th of the abdomen.
Shape, Size, and Colour
Shape
The liver is wedge shaped and resembles a 4-sided pyramid placed on 1 side with its base pointed in the direction of the right and apex steered in the direction of the left.
Weight
- In men: 1.4 to 1.8 kg.
- In females: 1.2 to 1.4 kg.
- In newborn: 1/18th of the body weight.
- At birth: 150 grams.
- Proportional weightIn grownup 1/40th of the body weight.
Colour
It’s reddish -brown in colour.
External Features
The wedge shaped liver presents 2 well defined surfaces, diaphragmatic and visceral and 1 well defined border, inferior border. The diaphragmatic surface is convex and extensive. It faces upwards, forwards, to the right and backwards. The visceral surface is comparatively flat and faces inferiorly. These 2 surfaces meet in front in the sharp inferior border. Conventionally the diaphragmatic surface is further subdivided into superior, anterior, right lateral, and posterior surfaces, however there’s no distinct difference between these surfaces.
Diaphragmatic Surface
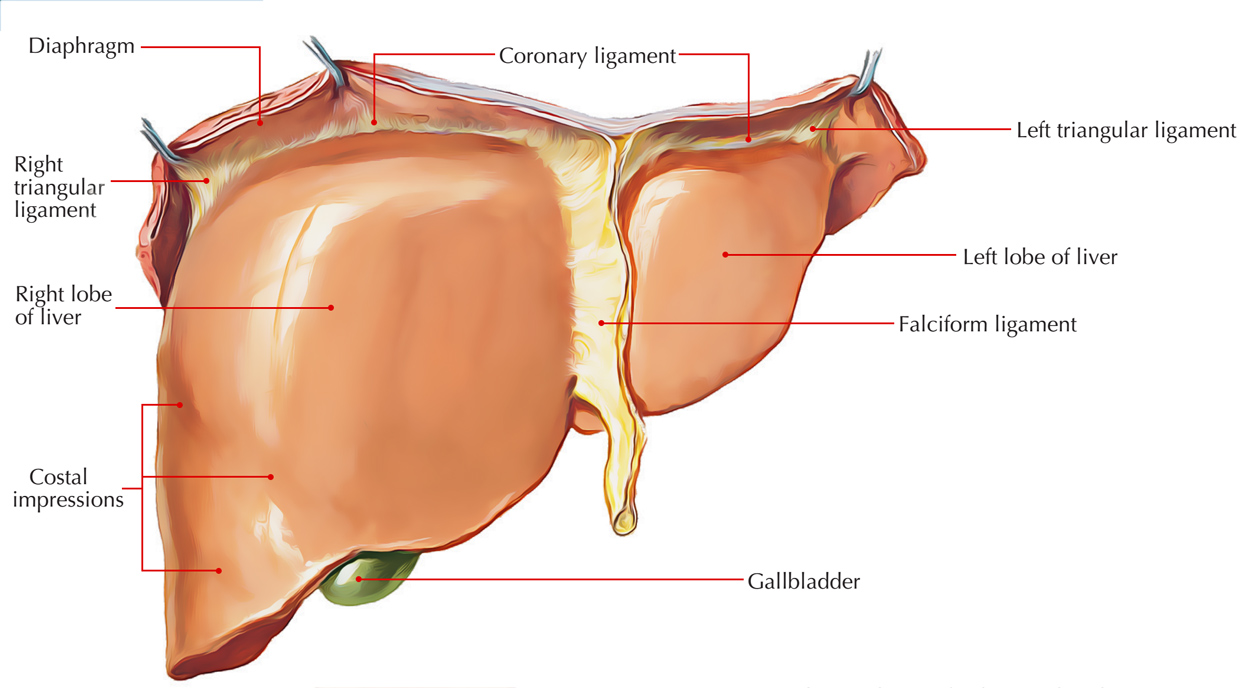
Liver: Diaphragmatic Surface
The dome-shaped diaphragmatic surface consists of smooth peritoneal regions which face superiorly, anteriorly and to the right and a rough empty area (devoid of the peritoneum) which faces posteriorly.
- The inferior vena cava (IVC) is embedded in the deep sulcus in the left part of the empty area. In many cases, this sulcus is roofed by the fibrous tissue referred to as ligament of IVC that might include hepatic tissue converting the sulcus into the tunnel.
- The peritoneal ligaments are coronary, right and left triangular and falciform ligaments.
Visceral Surface (Inferior Surface)
The visceral surface is comparatively flat or concave. It’s pointed downward, backward, and to the left. It’s divided in front from the diaphragmatic surface by the sharp inferior border and behind from the diaphragm by the posterior layer of coronary ligament. The remarkable features on the visceral surface are:
- Fossa for the gallbladder.
- Fissure for the ligamentum teres hepatis.
- Porta hepatis.
The visceral surface is covered by the peritoneum with the exception of at the fossa for gallbladder and the porta hepatis.
Remarkable Features on Diaphragmatic and Visceral Surfaces of the Liver
Surface | Features |
|---|---|
| Diaphragmaticsurface | A. Bare area of the liver |
| B. Groove for inferior vena cava | |
| C. Fissure for ligamentum venosum | |
| D. Attachment of coronary, right, and left triangular and falciform ligaments | |
| Visceral surface | A. Fissure for ligamentum teres hepatis |
| B. Porta hepatis |
Inferior Border
The features of the inferior border are as follows:
- It divides the diaphragmatic surface from the visceral surface.
- It’s rounded laterally where it separates the right lateral surface from the inferior surface.
- It’s sharp and thin medially where it divides the anterior surface from the inferior surface.
- It presents 2 notches:
1. Pass for ligamentum teres or interlobar notch: It’s situated just to the right of the median plane.
2. Cystic notch: It’s situated about 5 cm to the right of the median plane and frequently corresponds to the fundus of the gallbladder. - In the epigastrium, it goes from the right 9th costal cartilage to the 8th left costal cartilage, consequently it ascends sharply to the left.
- In the median plane, it is located in the transpyloric plane.
Lobes of The Liver
The lobes of the liver are classified into 2 types: (a) anatomical lobes and (b) physical (functional) lobes.
Anatomical Lobes
On the diaphragmatic surface, the liver is split into 2 lobes, left and right, by the connection of the falciform ligament. The right lobe which creates the base of the wedge-shaped liver is roughly 6 times bigger in relation to the left lobe.
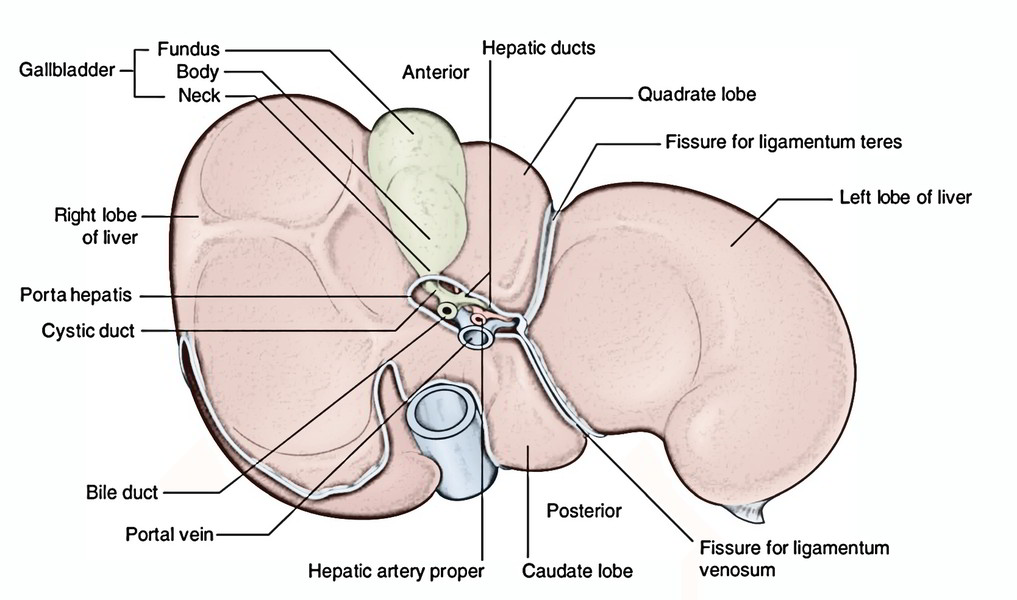
On the visceral surface, the liver is split into 4 lobes: (a) right lobe, (b) left lobe, (c) quadrate lobe, and (d) caudate lobe by fissures and fossae present on thissurface (Viz. fissures for ligamentum teres and ligamentum venosum, porta hepatis, groove of the IVC and fossa for the gallbladder). These fissures and fossae create an H-shaped shape.
- Right lobe to right of the fossa for gallbladder.
- Left lobe to the left of the fissures for ligamentum teres and ligamentum venosum.
- Quadrate lobe, between the fossa for gallbladder and the fissure for ligamentum teres below the porta hepatis.
- Caudate lobe, between the groove for IVC and the fissure for ligamentum venosum above the porta hepatis.
The anatomical lobes demarcated by surface features only function as useful landmarks however they’re not true lobes as they don’t correspond to the internal construction of the liver.
Physiological Lobes/Functional Lobes/True Lobes
The section of the liver into lobes is based upon the intrahepatic distribution of branches of the bile ducts, hepatic artery, and portal vein.
The liver is split into left and right physical lobes by an imaginary sagittal plane/line (Cantlie’s plane/line). On the posteroinferior surface this plane goes through the fossa for gallbladder, to the groove for IVC. (Notice: Caudate lobe is evenly shared between the left and right lobes.) On the anterosuperior outermost layer of the liver, this plane enters from the IVC to the cystic notch present a little to the right of the falciform ligament.
The physiological left and right lobes are roughly equivalent in size.
Every true lobe of the liver has its very own primary branch of the hepatic artery and portal vein and is emptied by its own hepatic duct.
Hepatic Sections (Sections of The Liver)
All these are structural units of the liver. There are 8 hepatic sections. They may be deduced as follows.
The right physical lobe is split into anterior and posterior parts, and the left bodily lobe into medial and lateral parts.
Every of these parts is further split into upper and lower parts and create 8 surgically resectable hepatic sections. The veins draining the hepatic sections are intersegmental, i.e., they drain more than 1 section.
On the surface of the liver, there’s no identifiable difference between anterior and posterior parts of the right lobe. The fissures for ligamentum teres and ligamentum venosum indicate the junction between the medial and lateral parts of the left lobe. The caudate and quadrate lobes are included into the upper and lower regions of the medial section of left lobe.
Couinaud’s segments: Based on nomenclature of Couinaud, the hepatic sections are numbered I to VIII, I to IV in the left hemiliver and V to VIII in the right hemiliver. According to this nomenclature, the section I corresponds to the caudate lobe and section IV corresponds to the quadrate lobe.
Section I to IV of the left lobe are supplied by the left branch of hepatic artery, left branch of portal vein and emptied by left hepatic duct. The sections V to VIII of right lobe are supplied by right hepatic artery, right branch of portal vein and emptied by right hepatic duct.
Clinical Significance
Segmental Resection of Liver
The hepatic sections aren’t well defined as the bronchopulmonary segments. The anatomy of hepatic sections is still of contentious utility in partial resection of the liver. For that reason, a true lobe instead of a section ought to be resected in many cases of partial hepatectomy.
A large volume of liver (80%) can be taken away safely because healthy hepatocytes have great ability of regeneration.
The liver can regrow to its initial size inside 6-12 months.
Peritoneal Relations
The majority of the liver is covered by the peritoneum. The regions that are not covered by the peritoneum are:
- Empty area of the liver: It’s a triangular area on the posterior aspect of the right lobe.
- Fossa for gallbladder, on the inferior outermost layer of the liver between right and quadrate lobes.
- Groove for IVC, on the posterior outermost layer of the right lobe of the liver.
- Groove for ligamentum venosum.
- Porta hepatis.
Ligaments
Ligaments of the liver are of 2 types: (a) false and (b) true.
Bogus Ligaments
The fictitious ligaments are in fact peritoneal folds and contain:
- Falciform ligament.
- Coronary ligament.
- Right triangular ligament.
- Left triangular ligament.
- Lesser omentum.
The caudate lobe is regarded as a different unique section by many authorities because it’s emptied by both left and right hepatic ducts and supplied by both left and right branches of the hepatic artery and portal vein.
Falciform Ligament
It’s a sickle-shaped fold of the peritoneum attaching the liver to the undersurface of the diaphragm and the anterior abdominal wall up to the umbilicus.
Coronary Ligament
- It’s a triangular fold of the peritoneum attaching the naked area of the liver to the diaphragm. It includes 2 layers- upper and lower. The upper layer is reflected from the diaphragm to the liver, on the other hand, the lower layer is reflected from the liver to the upper end of the kidney.
- When followed on the right side, the layers are constant with the right triangular ligament.
- When tracked on the left side, the upper layer is constant with the right layer of the falciform ligament and the lower layer is constant with the peritoneal reflection along the right border of the caudate lobe.
Right Triangular Ligament
It’s a small triangular fold of the peritoneum which attaches the right lateral surface of the liver to the diaphragm. It encloses the apex of the empty area of liver.
Left Triangular Ligament
It’s a very-very small triangular fold of the peritoneum which attaches the upper surface of the left lobe to the diaphragm.
- When followed to the left side, both layers come close to every other to create a free margin.
- When followed to the right side, the upper layer is constant with the left layer of the falciform ligament and the lower layer becomes continuous with the anterior layer of the lesser omentum along the left margin of the fissure for ligamentum venosum.
Lesser Omentum
It’s the fold of peritoneum attaching the smaller curvature of the stomach and proximal 1 inch (2.5 cm) of duodenum to the visceral surface of the liver. The hepatic connection is J-shaped with vertical limb being connected to the margins of fissure for ligamentum venosum and horizontal limb being connected to the margins/lips of porta hepatis.
True Ligaments
The true ligaments are really the remnants of fetal structures and contain:
- Ligamentum teres hepatis.
- Ligamentum venosum.
Ligamentum Teres Hepatis
It’s the remnant of the obliterated left umbilical vein and goes from the umbilicus to the left branch of the portal vein.
Ligamentum Venosum
It’s the remnant of the obliterated ductus venosus which in fetal life attaches the left branch of the portal vein together with the IVC.
Relationships
Diaphragmatic Surface
Superior Surface
- The convex left and right parts of the surface fit into the corresponding domes of the diaphragm, which divide them from the corresponding lung and pleura.
- The central depressed area of the surface is associated with the central tendon of the diaphragm, which divides it from the pericardium of the heart. Therefore, this area is usually referred to as cardiac belief.
Anterior Surface
It’s related to the xiphoid process and anterior abdominal wall in the median plane and diaphragm on every side. The falciform ligament is connected to this surface a little to the right of the median plane.
Right Lateral Surface
It’s related to the diaphragm opposite 7th to 11th ribs in the midaxillary line. Via the diaphragm:
- Upper one-third of this surface is related to both the lung and the pleura (remember the lung goes up to the 8th rib).
- Middle one-third of this surface is associated with the costodiaphragmatic recess of pleura (remember the pleura goes up to the 10th rib).
- Lower one-third of this surface is related to 10th and 11th ribs (i.e., it’s linked neither to the lung nor to the pleura).
For taking biopsy of the liver, the needle is added in the midaxillary line in 9th or 10th intercostal space to prevent injury to the lung.
Posterior Surface
This surface presents: bare area of the liver, groove for IVC, caudate lobe, fissure for ligamentum venosum, and posterior surface of the left lobe.
- The bare area of the liver is a triangular area to the right of groove for the IVC between the 2 layers of coronary and right triangular ligaments. It’s in direct contact with all the diaphragm. The right suprarenal gland is associated with the inferomedial part of the area, i.e., near the groove for IVC.
- The groove for IVC as the particular name signifies lodges the IVC. Its floor is pierced by the hepatic veins.
- The caudate lobe is linked to the superior recess of the lesser sac. The caudate lobe presents 2 processes: a papillary process, which originates from its left side, and a caudate process above the porta hepatis, which attaches it to the remainder of the liver.
- The fissure for ligamentum venosum is a deep cleft to the left of the caudate lobe. The ligamentum venosum is located in its floor.
- The posterior surface of the left lobe is associated with the abdominal part of the esophagus, just to the left of the upper part of fissure for ligamentum venosum and causes esophageal feeling. The fundus of the stomach is associated just to the left of the esophageal feeling.
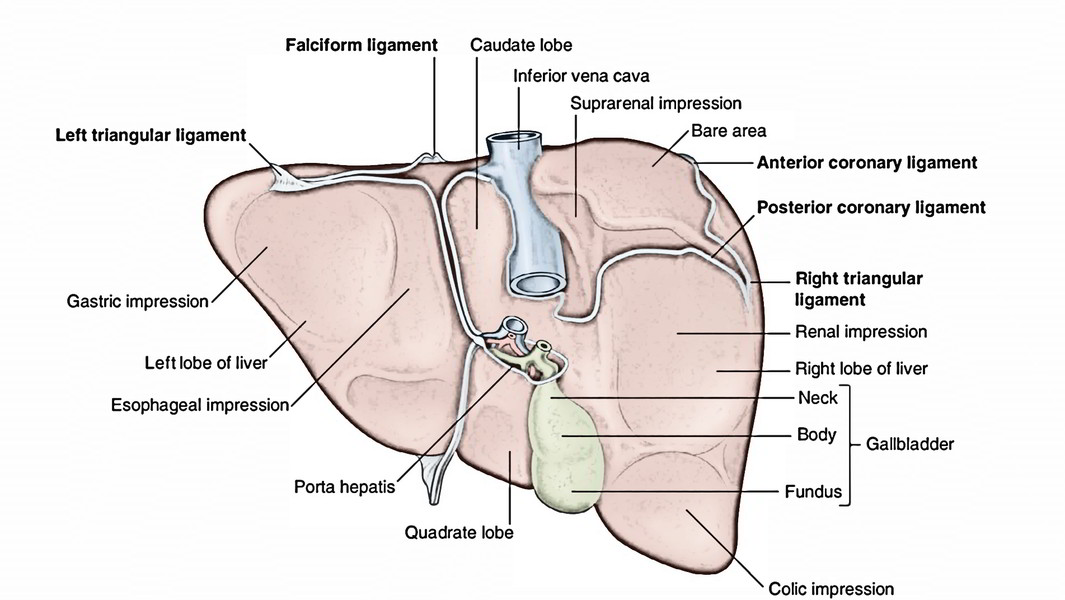
Visceral Surface (Inferior Surface)
- The inferior surface of the left lobe is associated with the anterosuperior outermost layer of the stomach, which generates a gastric perception. Near the left side of the fissure for ligamentum venosum, this surface presents a negligible elevation which arrives in touch together with the lesser omentum. For this reason, it’s named tuber omentale/omental tuberosity.
A) The fissure for ligamentum teres is a deep cleft to the left of the quadrate lobe. The ligamentum teres is located in its floor.
B) The inferior outermost layer of the right lobe presents 3 notable features: quadrate lobe, fossa for gallbladder, and porta hepatis. The Relations of the inferior surface are:
- The quadrate lobe is linked to the pyloric end of the stomach and the very first part of the duodenum.
- The fossa for gallbladder is located to the right of the quadrate lobe, inhabited by the gallbladder with its cystic duct near the right end of the porta hepatis.
- The right colic flexure is related to the inferior surface to the right of the gallbladder near the inferior margin and creates colic feeling.
- The junction of first and 2nd parts of the duodenum is related to the right upper part of the fossa for gallbladder and adjoining part of the right lobe and generates the duodenal impression.
- The right kidney is associated with the inferior surface posterior to the colic belief and to the right of the duodenal belief and causes renal feeling.
C) Porta hepatis (entrance of the liver) is a horizontal fissure on the inferior outermost layer of the liver between the quadrate lobe and the caudate lobe. The key structures going into the porta hepatis are left and right branches of the hepatic artery and portal vein, and the primary structures leaving the porta hepatis are left and right hepatic ducts. They are located in the arrangement from posterior to anterior as vein, artery, and duct (VAD). Also within the porta hepatis are lymph nodes and nerves of the liver.
Relationships of diaphragmatic and visceral surfaces of the liver.
Surface | Relations | |
|---|---|---|
| Diaphragmatic surface (parietal surface) | Superior surface with diaphragm intervening | 1. Corresponding lung and pleura on either side |
| 2. Pericardium and heart in the centre | ||
| Anterior surface | 1. Xiphoid process | |
| 2. Anterior abdominal wall | ||
| Right lateral surface with diaphragm intervening | 1. Lung and pleura in the upper one-third | |
| 2.Costodiaphragmatic recess in the middle one-third | ||
| 3. 10th and 11th ribs in the lower one-third | ||
| Posterior surface: | 1. Abdominal part of the esophagus | |
| 1. with peritoneum intervening | 2. Right suprarenal gland | |
| 2. with peritoneum not intervening | 3. Inferior vena cava | |
Clinical Significance
Surgical Significance of The Empty Area of The Liver
The bare area of the liver is indirect contact with the diaphragm, which divides it from the right pleural cavity. Surgically, it’s significant since it encloses the right extraperitoneal subphrenic space. In amoebic hepatitis, the pus may accumulate in this space and create a subphrenic abscess which may burst into the right pleural cavity via the diaphragm.
A potential anastomosis of venous capillaries exists in the region of bare area between the liver and the diaphragm. It becomes functional under certain pathological circumstances (example, portal hypertension).
Needle Biopsy of The Liver
In needle biopsy of the liver, the needle is added in the midaxillary line via 9th or 10th intercostal space. The needle goes through the chest wall, costodiaphragmatic recess of the pleura, diaphragm, and right anterior intraperitoneal space to goes into the liver. Needle fit above the 8th intercostalspace will injure the lung.
Blood Supply
The liver is a very vascular organ. It gets blood from 2 sources. The arterial blood (oxygenated) is supplied by the hepatic artery and venous blood (rich in nutrients) is supplied by the portal vein. In a normal mature (in the recumbent position), almost one-third of the cardiac output goes through the liver. About 80% of this is delivered via the portal vein and 20% is delivered via the hepatic artery.
Venous Drainage
Majority of the venous blood from liver is emptied by 3 large hepatic veins: (a) left hepatic vein between medial and lateral parts of the left true lobe, (b) middle hepatic vein between true left and right true lobes, and (c) right hepaticvein between anterior and posterior sections of the right true lobe. These veins don’t have the extrahepatic course. They come in the upper part of the groove for IVC and open directly in the IVC, just below the central tendon of the diaphragm. The 3 veins may goes into the IVC alone but the left and middle veins generally join, so that only 2 major veins join the IVC.
Points to be noticed
- The middle hepatic vein is located in the sagittal plane that divides the liver into true left and right lobes. Hence, it’s a useful landmark in radiological and ultrasonographic investigations.
- In addition to 3 large hepatic veins, several small accessory veins consisting of another vein from the caudate lobe issue in the lower part of the groove for IVC and open into the IVC.
- The hepatic veins are intersegmental (vide supra).
Lymphatic Drainage
A network of superficial lymphatics exists in the capsule of the liver underneath the peritoneum. The superficial lymphatics from the posterior aspect of the liver converge toward the empty area of the liver and convey with the extraperitoneal lymphatics which perforate the diaphragm and drain into the posterior mediastinal lymph nodes. The superficial lymphatics from the anterior aspect of the liverdrain into 3 or 4 nodes that are located in the porta hepatis (hepatic nodes). The nodes also get the lymphatics from the gallbladder. Efferents from these nodes run downward along the hepatic artery to coeliac nodes.
The lymphatics accompanying the portal triads represent the deep lymphatics. The deep lymphatics create 2 trunks. The ascending trunk enters the thorax via the vena caval opening and ends in the nodes around the IVC. The descending trunk empties in hepatic nodes found in the porta hepatis.
Nerve Supply
The liver is supplied by both sympathetic and parasympathetic fibres. The sympathetic fibres are originated from the coeliac plexus. They run along the vessels in the free margin of the lesser omentum and goes into the porta hepatis.
The parasympathetic fibres are originated from the hepatic branch of the anterior vagal trunk, which reaches the porta hepatis via the lesser omentum.
Pain happening because of distension of the hepatic capsule and hepatic peritoneum because of inflammation and swelling of the liver (hepatitis) run along the sympathetic fibres. The pain is frequently referred to the epigastrium and occasionally to the shoulder.
Variables Keeping The Liver in Position
All these are as follows:
- Hepatic veins attaching the liver to the IVC.
- Intra-abdominal pressure kept by the tone of abdominal muscles.
- Peritoneal ligaments attaching the liver to the abdominal walls.
Microscopic Structure
In a classical description, the liver includes hexagonal lobules (ancient liver lobules) created from anastomosing cords of hepatocytes radiating far from the central vein, a radicle of hepatic vein. At the periphery of the lobules in the corners of hexagon are portal triads/tracts. Every triad includes 3 structures viz. radicle of bile duct (hepatic ductal), hepatic artery (hepatic arteriole), and portal vein (portal venule). The plates/cords of hepatocytes are divided by vascular spaces referred to as sinusoids which attach the portal vein of the triad to the central vein of the lobule. The blood circulation in the sinusoids is from the periphery of the lobule toward the central vein.
The sinusoids interceding between the cords of hepatocytes are lined by endothelial cells, which present regular intercellular spaces/fenestrations. The fenestrations enable plasma (but not the blood cells) to leave the sinusoids and goes into the perisinusoidal spaces (spaces of Disse) between the endothelial lining and hepatocytes. Most of the cells of endothelial lining are able of phagocytic actions (Kupffer cells).
The bile produced by hepatocytes first enters the bile canaliculi situated between the opposite sides of adjacent hepatocytes. The bile canaliculi drain into the bile ductules of the portal triads which in turn unite to create the bigger intrahepatic ducts.
The portal triads are embedded in the perilobular connective tissue which pervades the liver and is constant with the capsule of the organ.
To study particular pathological circumstances, it’s useful to split liver into functional components termed portal vein lobules and hepatic acini.
- The portal lobule is a triangular unit/area of liver parenchyma bounded by 3 adjacent central veins. It consists of the portions of 3 ancient lobules with portal triad in the center.
- The liver acinus/hepatic acinus is a diamond-shaped unit/area of liver parenchyma. It contains portions of 2 ancient liver lobules with portal triad at every side of elliptical area and central vein on every end.
Development
The liver grows from a diverticulum (hepatic bud) from the distal end of the foregut. The hepatic bud elongates cranially and provides rise to a small accessory bud on its right side named pars cystica which creates cystic duct and gallbladder. The primary bud referred to as pars hepatica develops into the septum transversum. It bifurcates and provides rise to left and right hepatic ducts and liver parenchyma. The septum transversum includes the vitelline veins and umbilical veins before the hepatic bud invades it. These vessels subdivide to create sinusoids which invade the liver parenchyma breaking it up into hepatic cords. The bile canaliculi and ductules are created in the liver parenchyma and create links with the extrahepatic bile ducts at an afterwards period.
Clinical Significance
Cirrhosis of The Liver
The hepatocytes occasionally may go through necrosis following their injury and death caused by infection, toxins, alcohol, and poisons. The dead hepatocytes are replaced by fibrous tissue by the proliferation of the perilobular connective tissue. The resultant hepatic fibrosis is medically called cirrhosis of the liver. The patient develops jaundice as a result of blockage of bile flow. Resistance to blood flow via cirrhotic liver is raised which results in increase of pressure in the radicles of portal vein in the triads. Since portal vein and its tributaries are devoid of valves, the increased venous pressure in the portal vein causes engorgement and distension of all its tributaries, in addition to of spleen. This clinical condition is known as portal hypertension.
Extrahepatic Biliary Gear
The extrahepatic biliary gear gets the bile from liver, shops and concentrates it in the gallbladder, and carries it to the 2nd part of the duodenum when demanded.
It is composed of 5 parts:
- left and right hepatic ducts.
- Common hepatic duct.
- Gallbladder.
- Cystic duct.
- Bile duct (previously, common bile duct).
The anatomical understanding of the extrahepatic biliary equipment is incredibly significant medically because it’s frequently influenced in different disease processes like cholecystitis (inflammation of gallbladder), cholelithiasis (foundation of stones in the gallbladder), impediment of common bile duct (CBD), etc. Additionally, it’s often visualized by different imaging techniques.
Hepatic Ducts
The left and right hepatic ducts from the left and right lobes of the liver issue via porta hepatis and connect near its right end to create the common hepatic duct, which enters downward for about 2.5 cm (1 inch)and after that joined on its right side by the cystic duct to create the CBD. The angle between the cystic duct and the common hepatic duct is acute and is termed cystohepatic angle. In the right free margin of the lesser omentum, the common hepatic duct is located on the right side of the hepatic artery appropriate, in front of the portal vein. The accessory hepatic ducts are viewed in about 15% of cases. They generally come forth from right lobe of the liver and might open in 1 of the following sites: (a) common hepatic duct, (b) cystic duct, (c) bile duct, and (d) gallbladder.
Test Your Knowledge
Liver

 (70 votes, average: 4.34 out of 5)
(70 votes, average: 4.34 out of 5)