The spinal cord is the lower cylindrical part of the central nervous system inhabiting the upper two-thirds of the vertebral canal and is typically 45 cm long. It starts at the foramen magnum as the continuance of medulla oblongata and normally ends opposite the intervertebral disc between the L1 and L2 vertebrae. The spinal cord stretches up to the level of the lower border of S2 vertebra in foetus. The functions of the spinal cord are as follows:
- Transmission of info to and fro between body and brain.
- Performance of simple reflexes.
External Features
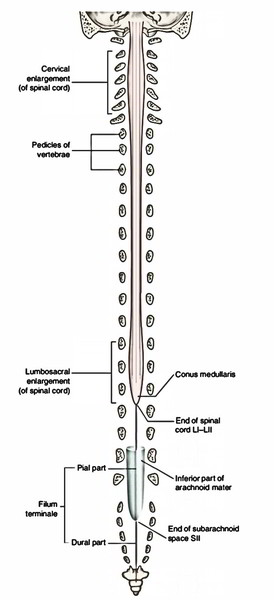
The spinal cord is cylindrical structure, somewhat flattened anteroposteriorly. Its lower end tapers into a cone creating the conus medullaris. The spinal cord supplies origin to 31 pairs of spinal nerves. The girth of spinal cord increases substantially in the regions that supply origin to large nerves of the limbs. These enlargements are called cervical and lumbar swellings/enlargements. The spinal cord presents the following external features:
- Fissures and sulci.
- Attachments of spinal nerve roots.
- Enlargements of the spinal cord.
Fissures and Sulci
The anterior aspect of spinal cord possesses a deep midline groove termed anterior median fissure. It stretches along the complete length of the spinal cord. On each side of anterior median fissure it presents anterolateral sulci. The posterior aspect of the spinal cord presents a shallow posterior median sulcus, from which a posterior median septum of neuroglial tissue extends into the substance of the cord to a varying extent.
Attachments of Spinal Nerve Roots
The anterior and posterior roots of the spinal nerve unify inside the intervertebral foramina. The anterior root is composed by 3 or 4 or rootlets, which come along the anterolateral sulcus of the spinal cord. The posterior root is composed by several rootlets that are connected to the posterolateral sulcus of the spinal cord. A short distance from the cord the rootlets unify to create one root. The anterior and posterior roots pass to their proper intervertebral foramina, where every evaginates dura mater individually before uniting to create the nerve trunk. The ganglion on the posterior root is located in the intervertebral foramen, inside the tubular evagination of dura and arachnoid proximal to the point of union of anterior and posterior nerve roots. At all levels from C1 to L1 vertebrae, the anterior and posterior nerve roots pass in front of and behind the ligamentum denticulatum, respectively. Since the spinal cord is shorter compared to the vertebral canal, the course of spinal nerve roots in the vertebral canal to get to the proper intervertebral foramen changes. The upper cervical nerve roots pass nearly horizontally, the thoracic nerve roots pass obliquely, while lumbar and sacral nerve roots descend just about vertically downwards creating the cauda equina. The cauda equina is a leash of lumbar (with the exception of L1), sacral and coccygeal nerve roots around the filum terminale in the pool of CSF. It’s thus called because the lower end of the spinal cord together with the aforementioned structures resembles the tail of a horse (cauda = tail, equina = horse).
Way Out of Spinal Nerves
All the spinal nerves leave out of vertebral canal via an intervertebral foramen with the exception of the following ones:
- C1 spinal nerve comes above the posterior arch of atlas vertebra.
- C2 comes between the posterior arch of atlas and axis vertebra.
- S5 and CX 1 come via lower end of the sacral canal. Other sacral nerves have different sacral foramina for every ramus.
Spinal Ganglia
All these are collection of nerve cell bodies of pseudounipolar neurons. The nerve cell bodies generate sensory fibres (peripheral processes) in the peripheral nerve and nerve fibres (central processes) in the dorsal root on which the ganglion is located. There is absolutely no synapse in the spinal ganglia. All the spinal ganglia are located in the intervertebral foramina with the exception of the sacral and coccygeal, which be located in the sacral canal and the very first 2 cervical, which be located in the corresponding position above and below the very first cervical vertebra, behind the articular facets. Spinal sections: The portion of spinal cord which supplies origin to a set of spinal nerves is referred to as spinal section. (The spinal sections aren’t observable on the surface.) Therefore the spinal cord is composed of 31 spinal sections. The size of section is dependent upon the amount of tissue supplied by every section. Because of relative shortening of the spinal cord as compared to the vertebral canal, the spinal sections is located above their corresponding vertebral level, a fact of great clinical value in figuring out the level of vertebral injury from signs and symptoms created as a result of injury to a certain section.
Enlargements of Spinal Cord
The spinal cord isn’t uniform in diameter. It presents 2 enlargements in those regions, which supply the upper and lower limbs and related girdles. The 2 enlargements are as follows:
- Cervical enlargement: In the region of C5 T1 spinal sections. The nerves originating from these sections create brachial plexus.
- Lumbar enlargement: In the region of L2 S3 spinal sections. The nerves originating from these sections create the lumbar plexus.
The vertebral levels of these enlargements are rather distinct from that of spinal sections, viz, cervical enlargement is located opposite C3 to T1 vertebrae and lumbar enlargement is located opposite T9 to L1 vertebrae. These enlargements in spinal cord are because of substantially increased mass of motor cells in the anterior horns of grey matter in these spinal sections. Approximate vertebral levels of the spinal sections
| Spinal segments | Vertebral levels |
|---|---|
| Cervical 1-8 | Foramen magnum to C6 vertebrae |
| Thoracic 1-6 | C6 - T4 vertebrae |
| Thoracic 7-12 | T4 - T9 vertebrae |
| Lumbar and sacral | T10 - L1 vertebrae |
Internal Structure
The spinal cord is composed of central mass of grey matter composed of nerve cells and peripheral mass of white matter composed of fibre tracts. In a cross section of the cord, the grey matter is viewed as an H-shaped (or butterfly shaped) fluted column, stretching through the length of the spinal cord It’s split into symmetrical left and right comma-shaped masses that are joined from the other side of the midline by a transverse gray commissure. The central canal of the cord goes through the centre of the gray commissure. The canal is encompassed by substantia gelatinosa centralis. The lateral comma-shaped mass of grey matter is split by a transverse gray commissure into a narrow elongated posterior horn and broad anterior horn. The posterior horn extends just about up to the face of the cord but anterior horn falls short of it. 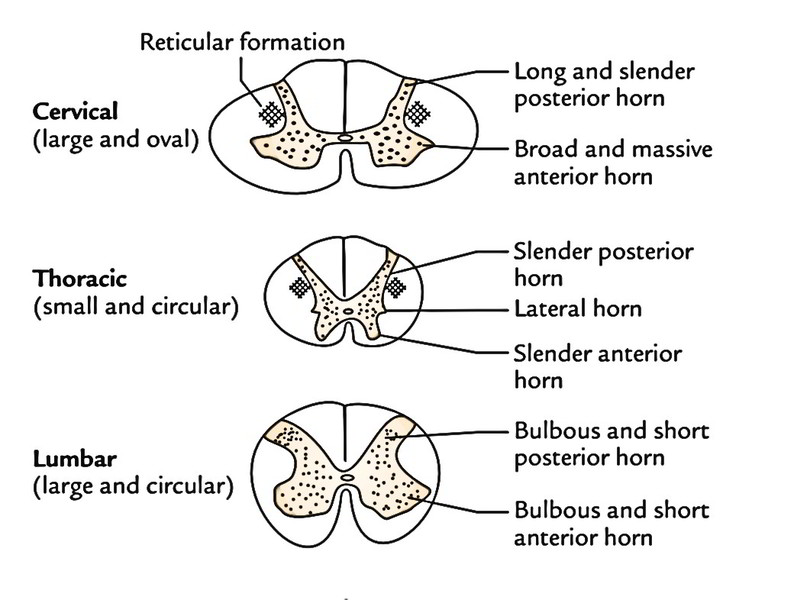
| Features | Levels | ||
|---|---|---|---|
| Cervical | Thoracic | Lumbar | |
| Grey matter | Large | Small | Large |
| Posterior horn | Slender and extends far posteriorly | Slender | Bulbous |
| Anterior horn | Massive | Slender | Bulbous |
| Lateral horn | Absent | Present | Present only in L1 and L2 segments |
| Reticular formation | Well developed | Poorly developed | Absent |
| Amount of white matter | Massive + + + + | Large (less than in the cervical region) + + + | Less (but slightly less than in the thoracic region) + + + |
Grey Matter
The grey matter of spinal cord is composed of (a) nerve cells, (b) neuroglia and (c) blood vessels.
Types of Neurons in the Grey Matter
Motor neurons: These exist in the anterior and lateral horns. Types of motor neurons in the anterior horn
- Alpha (a) neurons: They’re large multipolar cells (25 p, m or more in diameter) and supply the extrafusal skeletal muscle fibres.
- Gamma (y) neurons: They’re small multipolar cells (15-25 p, m in diameter) and supply the intrafusal muscle fibres of the neuromuscular spindles in skeletal muscles.
Types of motor neurons in the lateral horn: They’re preganglionic autonomic neurons.
- The axons of motor neurons leave the spinal cord as the last common path (Sherrington) via the ventral roots of the spinal nerves and reach the skeletal muscles.
- Sensory neurons: These are within the posterior horn and involved in relay of sensory info to the distinct parts of the brain creating ascending tracts; or to the other sections of spinal cord creating intersegmental tracts.
- Interneurons: These are small neurons present through the grey matter of the spinal cord.They attach different types of neurons, therefore also named association neurons. All these are either inhibitory or excitatory and concerned with integration of segmental actions.
Nerve Cell Groups in the Grey Columns of Spinal Cord
Cell Groups in the Anterior Grey Column
Numerous groups of motor neurons are seen in the cross section of anterior gray column, signifying several longitudinally ordered columns of varying lengths. They may be split into 3 major groups or nuclei: (a) medial, (b) lateral and (c) central.
- Medial group goes along the majority of the length of the spinal cord and innervate the axial musculature of the neck and trunk. This is further subdivided into ventromedial and dorsomedial parts.
- Sidelong group is confined to the cervical and lumbosacral enlargements and supply the limb muscles.
- Central group creates 3 clear nuclei that are pretty localized.
All these are as follows:
- Phrenic nucleus in the cervical region (going from C3 to C5 sections) innervates the diaphragm.
- Lumbosacral nucleus in the lumbosacral region (going from L2 to S3 sections), its function is unknown up to now.
- Spinal nucleus of accessory (XI cranial) nerve in the cervical region (going from C1 to C5 sections) and supplying origin to the spinal root of accessory nerve.
Cell Groups in the Posterior Grey Column
In the posterior gray column, the cell groups are ordered into 4 longitudinal columns; from the apex in the direction of the base they’re:
- Substantia gelatinosa (of Rolando).
- Nucleus proprius.
- Nucleus dorsalis (or Clarke’s column).
- Visceral afferent nucleus.
Substantia gelatinosa is situated in the apex of the posterior gray column and goes through the entire length of the spinal cord. It’s composed of small neurons (also named interneurons). It gets the afferent fibres of the lateral section of the posterior nerve roots carrying chiefly, the pain and temperature sensations. Several of those fibres synapse with the interneurons of substantia gelatinosa. The substantia gelatinosa is continuous above with the nucleus of spinal tract of the trigeminal nerve. Nucleus proprius is a group of large nerve cells situated anterior to the substantia gelatinosa and makes up the primary majority of cells existing in the posterior grey column. It stretches along the entire length of the spinal cord and gets the fibres from posterior white column that are connected with the awareness of position and movement (proprioception), 2 -point discrimination and shaking. Nucleus dorsalis (Clarke’s column) inhabits the medial part of the base of the posterior grey column, projecting somewhat into the posterior funiculus and stretches from C8 to L2/L3 sections of the cord and gets proprioceptive afferents (muscle and joint perception) and exteroceptive afferents (touch and pressure from the trunk and lower limb). Visceral afferent nucleus lies lateral to the nucleus dorsalis and stretches from T1 to L2 and from S2 to S4 sections of the cord and gets visceral afferents from the dorsal nerve roots.
Cell Groups in the Intermediate (Lateral) Grey Column
The cells of the lateral grey column create 2 nuclei: (a) intermediolateral and (b) intermediomedial.
- The intermediolateral nucleus goes from T1 to L2 sections of the cord and supplies origin to preganglionic fibres of the sympathetic nervous system (thoracolumbar outflow) which make the cord together with the anterior nerve roots.
- The intermediomedial nucleus goes from S2 to S4 sections of the cord and supplies origin to preganglionic fibres of parasympathetic nervous system (sacral outflow), which also pass out via the anterior nerve roots of the corresponding sacral nerves.
Besides the central grey matter, there are strands of grey matter in the lateral white column adjacent to the base of the posterior horn called reticular formation.
White Matter
The white matter of the spinal cord encompasses the central H shaped mass of grey matter and primarily is composed of nerve fibres, the large percentage of them being myelinated, supplying it a white look. In every half of the spinal cord, the white matter is split into 3 parts referred to as columns:
- Posterior white column, between the posterior median septum and the posterior horn.
- Lateral white column, between the anterior and posterior horns.
- Anterior white column, between the anterior median fissure and the anterior horn.
The anterior white columns are joined together by the white commissure. Every white column is created from tracts that are either ascending (sensory) or descending (motor). Generally, the posterior white column is sensory, the anterior column is motor and lateral column is combined (i.e., motor as well as sensory). Farther, the ascending tracts are found in the direction of the periphery and the descending tracts in the direction of the centre.
Tracts of The Spinal Cord
The tracts are defined as collections of nerve fibres inside the central nervous system, which have same origin, course and conclusion. They’re occasionally known as fasciculi (= bundles) or lemnisci (= ribbons). The tracts are called after the names of masses of grey matter linked by them. Their names normally include 2 parts (or terms), the very first term indicates the origin and second the conclusion of the tract. For instance, a tract originating in cerebral cortex and ending in the spinal cord is referred to as corticospinal tract. Likewise a tract originating in the spinal cord and ending in the thalamus is referred to as spinothalamic tract.
Arterial Supply
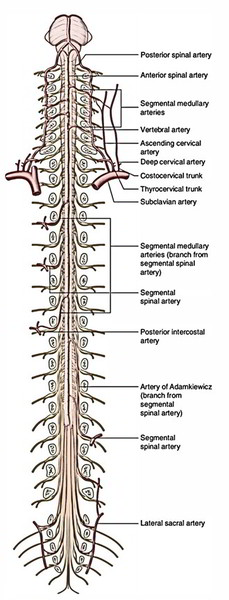
- Anterior spinal artery
- Posterior spinal arteries
- Segmental arteries
Anterior Spinal Artery
The anterior spinal artery is composed by the joining of 2 small spinal branches of the left and right vertebral arteries in the upper cervical canal. It runs caudally in the anterior median fissure of the spinal cord and ends along the filum terminale.
Posterior Spinal Arteries
- There are just two posterior spinal arteries every appearing as a small branch from either the vertebral or posterior inferior cerebellar artery. Every posterior spinal artery runs down on the posterolateral aspect of the cord in the posterolateral sulcus along the line of connection of posterior nerve roots and generally splits into 2 collateral arteries along the medial and lateral side of the posterior nerve roots. Consequently there are 5 longitudinal arteries around the spinal cord.
- These arteries are bolstered by the segmental arteries (feeder arteries) to create 5 longitudinal arterial trunks. These arterial trunks convey around the cord creating a pial plexus, the vasocorona/arteriae coronae. The arteriae coronae supply peripheral branches, which supply the superficial regions of the cord.
- The anterior spinal artery supplies the anterior two-third of the cord, while 2 posterior spinal arteries collectively supply the posterior one-third of the cord.
Segmental Arteries
The segmental arteries are spinal branches of deep cervical, ascending cervical, posterior intercostal, lumbar and lateral sacral arteries. They reach the spinal cord as the anterior and posterior radicular arteries along the corresponding roots of the spinal nerves, respectively. They primarily nourish the nerve roots. The largest segmental (radicular) arteries at the 1st (T1) and 11th thoracic (T11) segmental levels are frequently called arteria radicularis magna (arteries of Adamkiewicz).
Clinical Significance
Anterior Spinal Artery Syndrome
It happens because of occlusion (thrombosis or compression of the anterior spinal artery). Since the anterior spinal artery supplies anterior two-third of the cord, the occlusion of the artery will lead to these signs and symptoms:
- Motor symptoms because of participation of corticospinal tracts and anterior grey columns.
- Sensory symptoms (viz. bilateral loss of pain and temperature sense) because of ischemia of spinothalamic tracts.
The conscious proprioceptive sensations are maintained as the region of posterior white column is supplied by posterior spinal arteries.
Venous Drainage
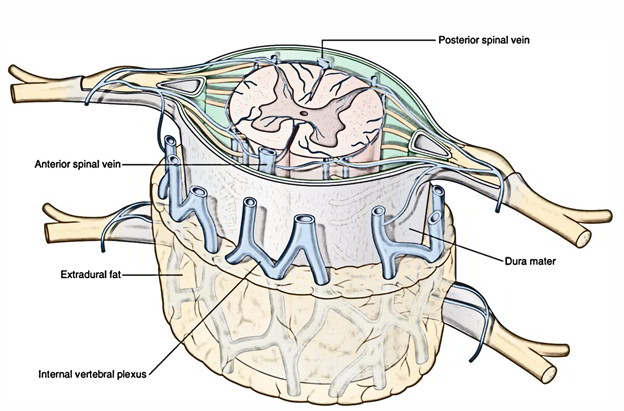
- 2 median longitudinal, 1 in the anterior median fissure and the other in the posteromedian sulcus.
- 2 anterolateral, 1 on either side, posterior to the anterior nerve roots.
- 2 posterolateral, 1 on either side, posterior to the posterior nerve roots.
These longitudinal venous channels convey with all the internal vertebral venous plexus and emptied by veins, which make via the intervertebral foramina to empty into the vertebral, posterior intercostal, lumbar and lateral sacral veins. The internal vertebral venous plexus conveys above with the basilar venous plexus.

 (60 votes, average: 4.77 out of 5)
(60 votes, average: 4.77 out of 5)